
Facts About Degenerative Disc Disease and Sciatica
Back pain can be a number of different things. Find out some facts regarding degenerative disc disease and sciatica.

3 Signs You Have a Slipped or Bulging Disc
When a disc in your lower spine bulges or tears, you may feel pain in your lower back and/or your leg. Here are 3 unique signs of a herniated or protruding disc to help you identify the underlying cause of your lower back problem.

Cervical Disc Surgery: Disc Replacement or Fusion?
Article featured on WebMD, medically reviewed by Sabrina Felson,…

Understanding Spinal Disk Problems — the Basics
Article Featured on WebMD
What Are Spinal Disk Problems?
Anybody…
Lumbar Spine Surgery
Article Featured on Spine Health
Lumbar surgery refers to…
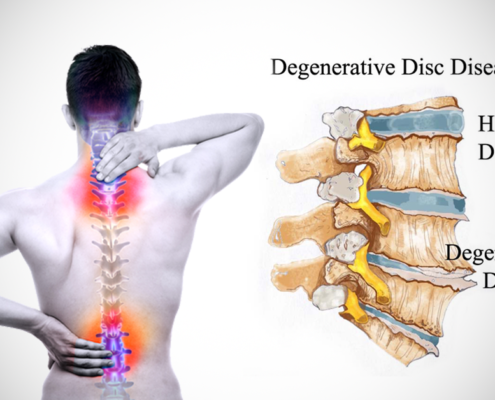
What Is Degenerative Disc Disease?
By Brian McHugh, MD | Featured on Spine Health
Degenerative…
How to tell if you have a Herniated Disk
Article Featured on AAOS
A common source of back or neck pain…
