
Could Your Foot Pain Be Caused by a Problem in Your Spine?
This blog provides a list of common causes of foot pain and helpful pointers to help you understand the origin of your foot pain.

Hip-Spine Syndrome: It’s Complicated (and Often Overlooked)
A patient with hip arthritis may experience hip or groin pain as well as trouble walking, while a patient with lumbar spinal stenosis may have pain down their leg, or neurologic symptoms such as numbness, tingling, or weakness.

How to Protect Your Spine as You Age
The human spine consists of discs and joints that, like a hinge on a door, can wear out with time. While you may hear worrying terms such as “degeneration” or “arthritis” to describe these changes, it’s a natural part of the aging process.

5 Benefits Of Aquatic Therapy For Spine Pain
The pool is a great place to take your workouts or physical therapy exercises. Here’s a look at five reasons why your back benefits from aquatic therapy.

When to Turn to Spine Surgery When Nothing Else Will Do
A surgical option may be the best way to fix the problem and get long-term relief.

Keeping Your Spine Healthy
Article featured on Brigham Health Hub
While the COVID-19 pandemic…

How to Protect Your Spine When You Have Osteoporosis
Article featured on Spine-Health
In some cases of osteoporosis,…

Spine Structure and Function
Article featured on the Cleveland Clinic
Key parts of…

Cervical Disc Surgery: Disc Replacement or Fusion?
Article featured on WebMD, medically reviewed by Sabrina Felson,…
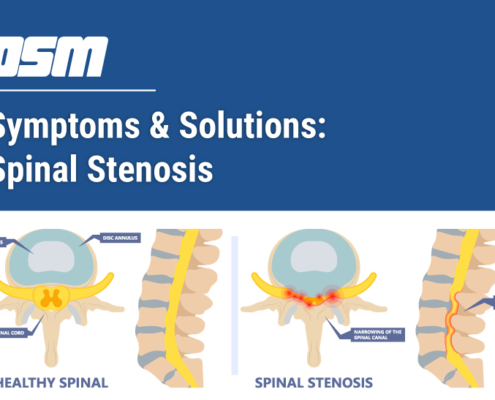
Symptoms & Solutions: Spinal Stenosis
Article featured on Arkansas Surgical Hospital
What is Spinal…
